Topics: Atherosclerosis, Diabetes, Gangrene
 Many people are unaware of the connection between diabetes and gangrene. However, education on these topics are very important because it can be the different between life and limb.
Many people are unaware of the connection between diabetes and gangrene. However, education on these topics are very important because it can be the different between life and limb.
Gangrene can quickly create a need for limb amputation if it is not diagnosed and treated within time. Patients with diabetes need to be aware of the symptoms of gangrene and understand why they are at a greater risk of developing it.
What is Gangrene?
In order to better understand the connection between diabetes and gangrene, it is first important to understand what gangrene is. Gangrene is a condition where the skin and soft tissue on a particular area of the body begins to die because of a lack of healthy blood flow.
Gangrene is typically found on areas of the body like the fingers, toes, hands and feet because these extremities - the furthest point - are furthest distance the heart has to pump blood. In addition, they are more likely to receive the least blood flow if there is an obstruction in the artery.
What Symptoms of Gangrene Should Patients with Diabetes Look For?
As previously stated, it is important for patients with diabetes to be aware of the signs and symptoms of gangrene so they can catch it early.
The primary symptoms of gangrene are:
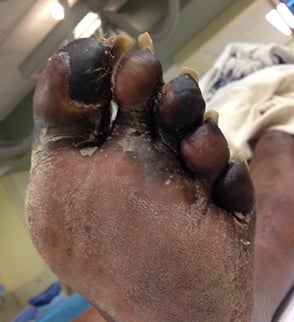
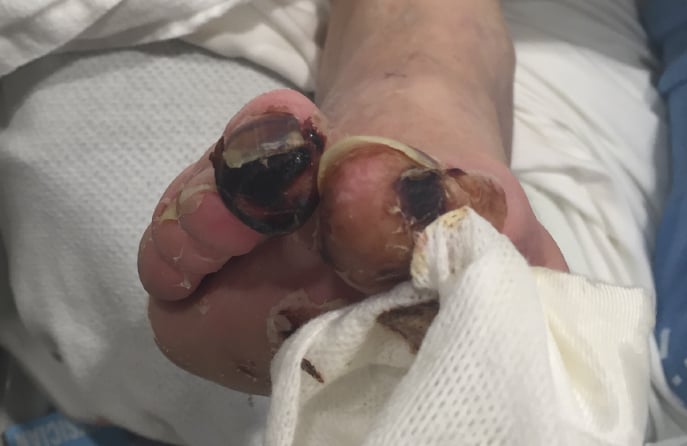
- The loss of color in the body part that is affected
- The area will change from a red color to black
- The skin will change in appearance to look shiny and will start shedding.
- The affected area may become painful to the touch
- The pain of the gangrene will eventually transition to the loss of sensation and ultimately result in tissue death
Diabetes and Gangrene: What’s the Link?
Patients with diabetes are likely to develop gangrene because they are more likely to develop Peripheral Artery Disease (PAD). The connection is so strong, in fact, that patients with diabetes are four times more likely to develop PAD. Additionally, out of all of the symptomatic patients with Peripheral Artery Disease, 40% of them had diabetes.1
Peripheral Artery Disease, Diabetes and Gangrene
One of the most important connections between diabetes and gangrene is PAD. Peripheral Artery Disease is a disease in which patients have poor circulation caused by atherosclerosis in the arteries.
Atherosclerosis in the artery
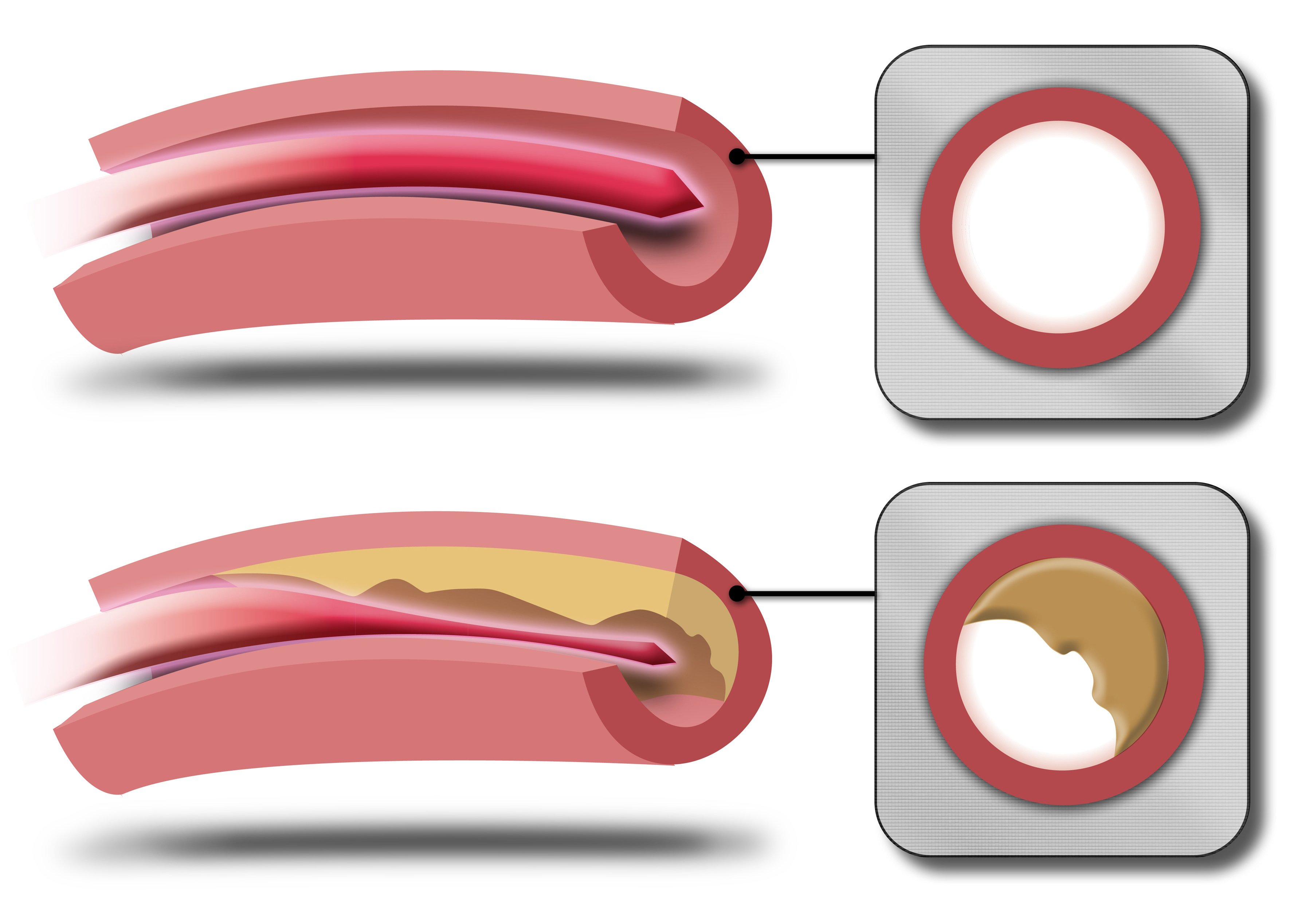
Atherosclerosis essentially causes plaque to buildup in the arteries which blocks the healthy blood flow which causes patients with diabetes and Peripheral Artery Disease to have poor circulation. As previously mentioned, this poor circulation can become very dangerous for patients very quickly. If patients with diabetes and PAD cannot reestablish healthy blood flow they may develop gangrene.
As Peripheral Artery Disease typically affects the feet of patients, the gangrene most commonly is found on the feet. However, this can be dangerous because patients with diabetes may experience diabetic neuropathy.
This is a type of nerve damage where patients with diabetes experience a numbness in their legs and feet. If diabetic patients have undiagnosed Peripheral Artery Disease they may miss the painful symptoms of gangrene because of diabetic neuropathy and would not know they have gangrene until it is too late and amputation is the only solution left.
What Should Patients with Diabetes do to Treat Gangrene?
Check Your Feet
Patients with diabetes are at risk of developing gangrene. Therefore, if you have diabetes, it is important that you examine your feet daily for early signs of gangrene.
This is a helpful preventative measure because you will be able to see physical signs of gangrene even if you can’t feel it due to neuropathy. If you notice any grey or black tissue on your feet make sure that you seek medical attention immediately.
Restoring Blood Flow
Restoring blood flow, also known as revascularization, is critical to restoring blood flow and saving the limb. In one study that looked at survival rates of diabetic patients concluded, “revascularization is the best therapy to eliminate pain and heal foot lesion in patients with Critical Limb Ischemia (the worst form of PAD).2
Today there is cutting edge technology to restore blood flow in diabetic patients and reverse the symptoms of gangrene. This technology is known as “Lumivascular” since it allows your doctor to see inside the artery and precisely remove the plaque that is obstructing the artery and preventing healthy blood flow.
Lumivascular atherectomy – Seeing inside your vessel
A Lumivascular atherectomy uses a camera to generate real time imaging inside the artery. Throughout the atherectomy, your doctor will be able to discern between healthy artery walls and plaque so they won’t harm the healthy tissue while removing plaque and diseased tissue. The goal of a Lumivascular atherectomy is to restore healthy blood flow, improve the patient’s circulation and ultimately reverse the symptoms of gangrene.
Seeing is believing – Gangrene Before and After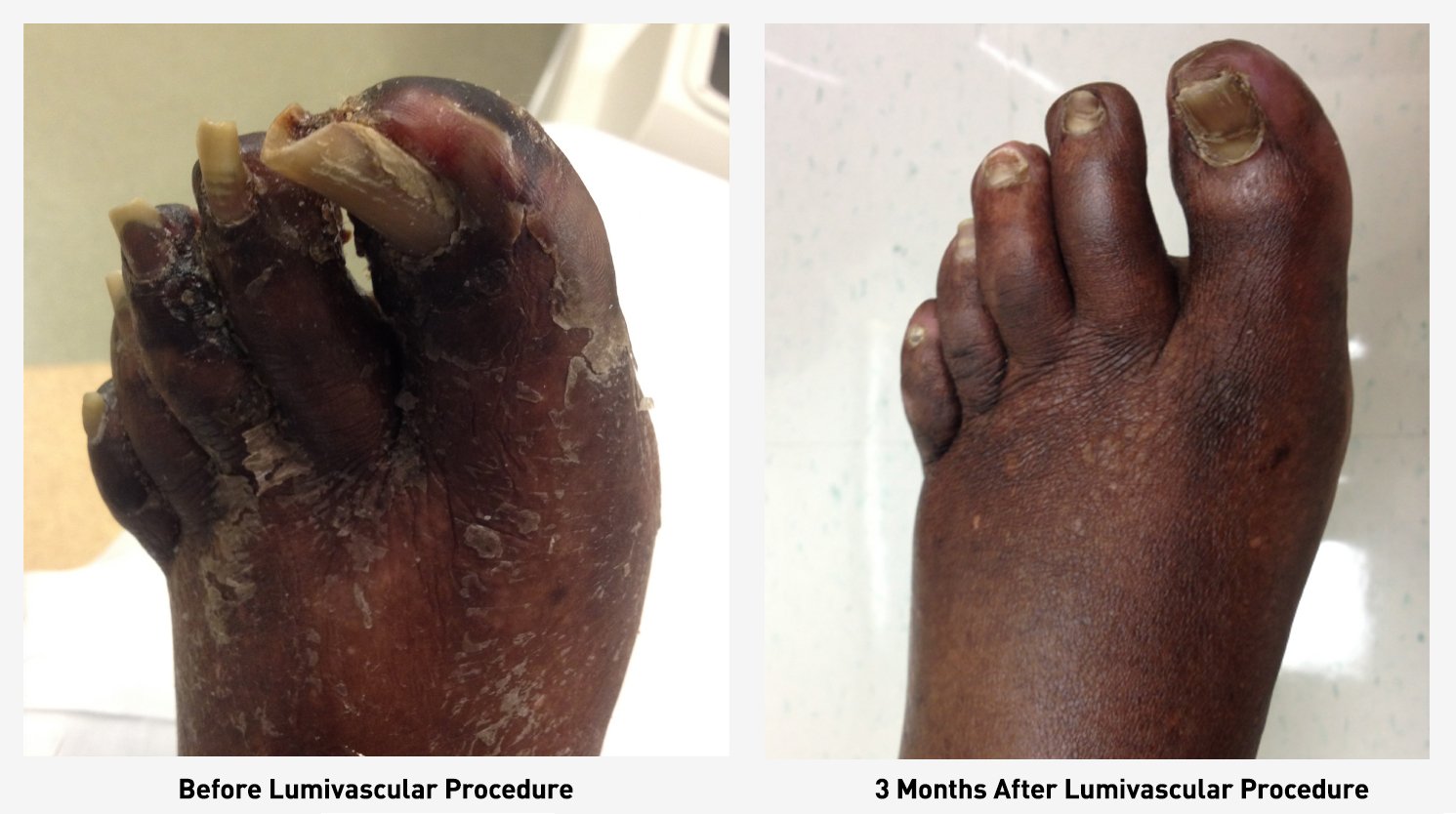
If you have developed gangrene due to diabetes and PAD, a Lumivascular atherectomy may be the best treatment option for you. Be sure to ask your doctor if the Lumivascular atherectomy could work for you. Click here to find a Lumivascular atherectomy physician nearest you.
Helpful resources:
- PAD Patient Guide – our eBook will explain what PAD is and how to treat it.
- PAD Patient Webinar – In depth presentation from Dr. Jaafer Golzar
- Patient Stories – Watch how patients like you have overcome their symptoms.
- Find a Doctor – Find a Lumivascular Doctor near you.
If you have found this article helpful, please don’t forget to share!
References:
- Hingorani, et al. The management of diabetic foot: A clinical practice guideline by the Society for Vascular Surgery in collaboration with the American Podiatric Medical Association and the Society for Vascular Medicine. J Vasc Surg 2016;63:3S-21S
- Faglia, et al. Early and Five-year Amputation and Survival Rate of Diabetic Patients with Critical Limb Ischemia: Data of a Cohort Study of 564 Patients. Eur J Vasc Endovasc Surg 32, 484e490