Topics: Peripheral Artery Disease, Atherectomy, Diabetes, Leg pain, Amputation, PAD Awareness Month, PAD Diagnosis, PAD, sleep
Sleep is an essential part of our daily life, influencing our overall health and well-being. Sleep also has a significant impact on cardiovascular health. Adequate and good quality sleep is crucial for maintaining a healthy cardiovascular system. Insufficient sleep or poor-quality sleep can increase the risk of developing cardiovascular conditions like hypertension, coronary artery disease, stroke, irregular heart rhythms, and Peripheral Artery Disease (PAD).1

What is PAD?
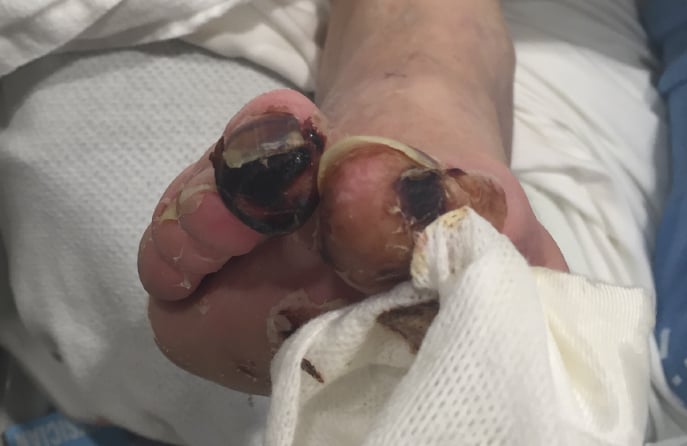
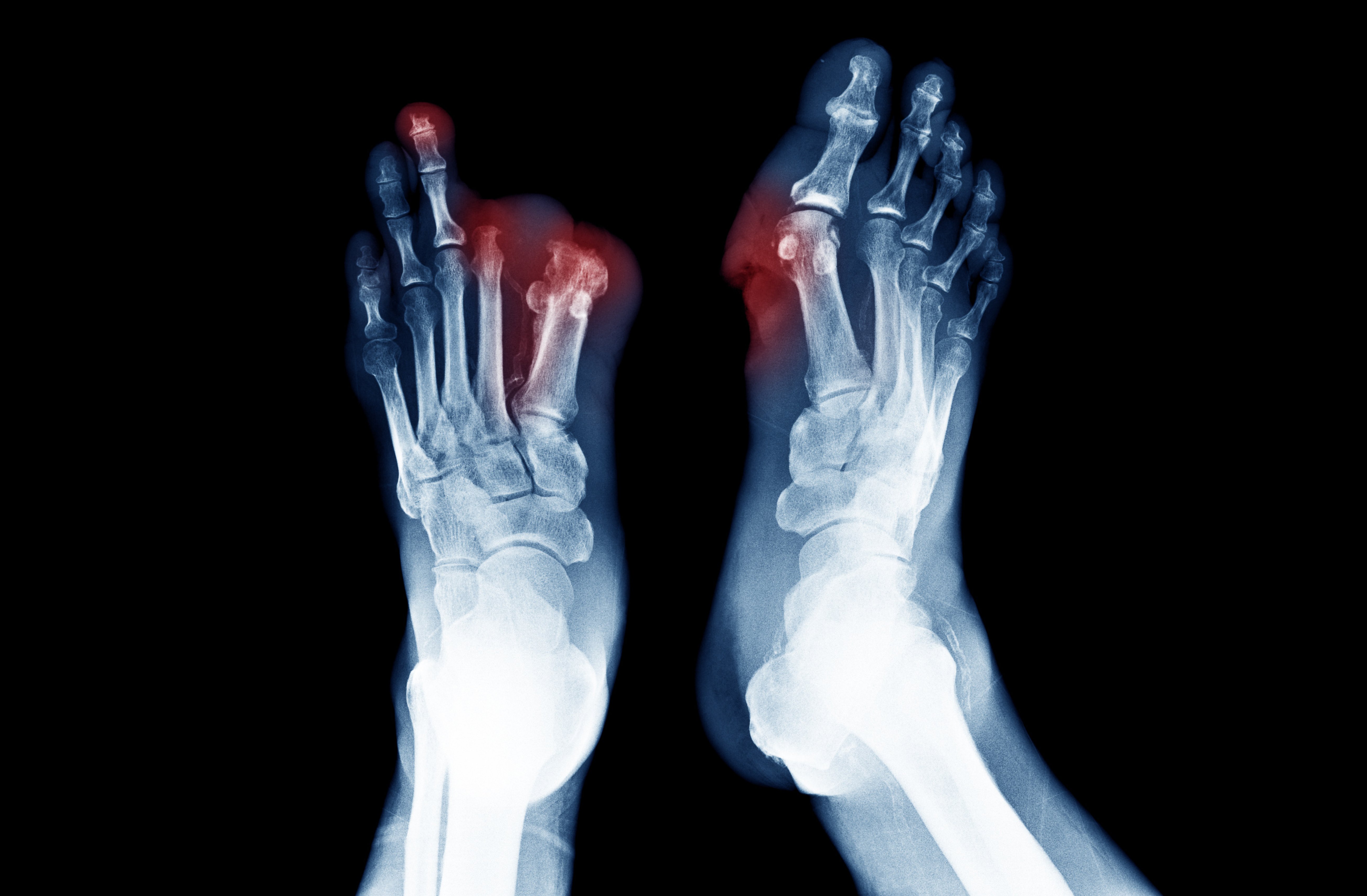
PAD is a common circulatory disorder characterized by the narrowing or blockage of arteries that supply blood to the limbs, typically the legs. This narrowing is often caused by a buildup of fatty deposits (plaques) in the arterial walls, leading to reduced blood flow. As a result, individuals with PAD may experience symptoms such as leg pain, cramping, or weakness during physical activity, which is known as intermittent claudication. If left untreated, PAD can lead to more severe complications and increase the risk of cardiovascular events. Early detection and appropriate management are crucial to improve symptoms and reduce the risk of complications.
Sleep disturbances can disrupt hormone balance, impair blood vessel function, and contribute to conditions like insulin resistance and obesity, which are risk factors for heart disease. Prioritizing sufficient and restful sleep is essential for maintaining healthy blood pressure, inflammation levels, and hormone balance, promoting a healthier heart and reducing the risk of cardiovascular disease.1
Dr. Shuai Yuan of the Karolinska Institute, Stockholm, Sweden aimed to investigate the correlation between sleep and cardiovascular health. Dr. Yuan highlighted that peripheral artery disease (PAD) affects over 200 million individuals worldwide. "Our study suggests that sleeping for seven to eight hours a night is a good habit for lowering the risk of PAD […] Insufficient night-time sleep and daytime napping have previously been associated with a raised risk of coronary artery disease which, like PAD, is caused by clogged arteries. In addition, sleeping problems are among the top ranked complaints in PAD patients. There are limited data on the impact of sleep habits on PAD and vice versa, and our study aimed to fill that gap."2
The research involved over 650,000 participants and was divided into two phases. Initially, the scientists investigated the connections between sleep duration, daytime napping, and the risk of PAD. In the subsequent phase, they utilized genetic data to conduct naturally randomized controlled trials, known as Mendelian randomization, to explore the causal relationships between these factors.2
Mendelian randomization
Mendelian randomization (MR) is a statistical method that uses randomly distributed genetic variants present from birth to determine causal relationships between factors. By linking these genetic clues to specific outcomes like diseases, scientists can better understand causation rather than coincidence. MR is valuable for uncovering how things work and guiding disease prevention or treatment interventions. Still, researchers must consider its limitations and assumptions during analysis.
The Research
The study, reported in the European Society of Cardiology, investigated the relationship among sleep duration, daytime napping, and PAD risk using both observational and Mendelian randomization (MR) analyses.1 The researchers gathered data from three cohorts: the Swedish Infrastructure for Medical Population-based Life-course and Environmental Research (SIMPLER), the Veterans Affairs Million Veteran Program (MVP), and the UK Biobank.
It is essential to note that no single study can definitively prove causality. While the MR analysis provided strong evidence for a causal relationship, further research is needed to corroborate these findings and explore potential underlying mechanisms.
"Observational analyses are limited by reverse causality” Dr. Yuan said, “meaning that if an association between sleep habits and PAD is found, we cannot be certain if sleep habits caused PAD or having PAD caused the sleep habits. Mendelian randomization is a robust method for evaluating causality and provides more certainty about the results."2
Upon careful analysis of the data, the researchers discovered a U-shaped curve association between sleep duration and Peripheral Artery Disease (PAD). Surprisingly, both short sleep durations (less than 5 hours) and long sleep durations (more than 8 hours) were found to be linked to an increased risk of developing PAD, emphasizing the potential impact of sleep patterns on cardiovascular health.1
To strengthen their findings, the researchers employed Mendelian Randomization (MR) analyses, which confirmed the results obtained from the observational studies and suggested a potential causal relationship between short sleep duration and an increased risk of PAD. This indicates that individuals genetically predisposed to shorter sleep durations may face a higher likelihood of developing PAD, adding to the understanding of genetic factors influencing sleep duration and its impact on cardiovascular health.1
The significance of sleep in maintaining cardiovascular well-being cannot be overstated, as the study's results bring new insights to sleep’s effect on cardiovascular health. It emphasizes the need for prioritizing sufficient and restful sleep to mitigate the risk of PAD and other cardiovascular conditions. Remarkably, each 1-hour increase in genetically predicted sleep duration was associated with a 30% decrease in the risk of PAD, suggesting that longer sleep durations within a genetically determined range may have a protective effect against PAD development.1
Future Directions and Action Steps
This study provides valuable insights into the link between sleep habits and PAD risk, emphasizing the significance of healthy sleep patterns for cardiovascular well-being. By uncovering potential genetic influences on sleep duration and its impact on PAD, the research paves the way for further investigation and potential sleep-related interventions to enhance cardiovascular health. These findings have significant implications for PAD management, suggesting that addressing sleep duration and quality could be a crucial aspect of treatment.
Integrating sleep-related interventions into the treatment plan may complement existing therapies and optimize cardiovascular health for individuals with PAD. Additionally, personalized treatment plans tailored to individual sleep patterns could be developed, considering genetic predispositions to sleep duration to optimize cardiovascular health. Recognizing the impact of healthy sleep patterns on cardiovascular health allows healthcare providers to potentially improve outcomes and enhance the effectiveness of traditional treatment options for PAD.

How Do You Treat Peripheral Artery Disease?
The treatment for Peripheral Artery Disease (PAD) aims to manage the symptoms, improve blood flow, and reduce the risk of complications. The specific treatment options depend on the severity of the condition and individual patient factors. Here are some common treatments for PAD:
- Lifestyle Changes: Lifestyle modifications play a crucial role in managing PAD. These may include:
- Smoking cessation: Quitting smoking is essential as smoking worsens PAD and increases the risk of complications.
- Exercise: A supervised exercise program, such as walking, can help improve circulation and reduce symptoms.
- Healthy diet: A balanced diet low in saturated fats and cholesterol can help control other risk factors, such as high blood pressure and cholesterol levels.
- Weight management: Maintaining a healthy weight reduces stress on the arteries and improves blood flow.
- Medications: Various medications may be prescribed to manage PAD and its related risk factors, such as:
- Antiplatelet agents: Medications like aspirin or clopidogrel may be prescribed to reduce the risk of blood clots and improve blood flow.
- Cholesterol-lowering drugs: Statins are often used to manage high cholesterol levels and reduce the risk of atherosclerosis progression.
- Blood pressure medications: These drugs help control hypertension and reduce stress on the arteries.
- Peripheral Angioplasty: This is a minimally invasive procedure used to widen narrowed or blocked arteries. A small balloon catheter is inserted into the affected artery and inflated to open the narrowed section. Sometimes, a stent may be placed to keep the artery open.
- Peripheral Arterial Bypass Surgery: In severe cases, when other treatments are ineffective, bypass surgery may be recommended. A blood vessel graft is used to create a detour around the blocked or narrowed section of the artery, restoring blood flow to the affected area.
- Endarterectomy: In this surgical procedure, the plaque buildup inside the affected artery is removed, improving blood flow.
- It involves removing the inner lining of the affected artery along with the plaque buildup.
- Endarterectomy is commonly performed on larger arteries, especially those closer to the heart, such as the carotid arteries in the neck, to treat carotid artery disease.
- During the procedure, a surgeon makes an incision in the artery, exposes the plaque, and carefully removes it along with the inner layer of the artery.
- The artery is then repaired, and the incision is closed.
- Thrombolytic Therapy: This treatment involves using medications to dissolve blood clots that may be causing a blockage in the artery.
- Atherectomy: A minimally invasive procedure used to remove plaque buildup (atherosclerosis) from narrowed arteries. It involves using a specialized catheter with cutting or grinding devices to physically remove or break up the plaque, restoring blood flow through the affected artery.
- Directional Atherectomy: The catheter has a rotating blade at the tip, which cuts and removes the plaque from the arterial wall.
- Rotational Atherectomy: This technique uses a high-speed rotating burr at the catheter's tip to grind away the plaque.
- Orbital Atherectomy: The catheter has a diamond-coated crown that rotates eccentrically to sand the plaque and open up the artery.
It is crucial for individuals with PAD to work closely with their healthcare providers to develop a personalized treatment plan. Early diagnosis and appropriate management can help improve quality of life, reduce symptoms, and prevent complications associated with PAD.
What Avinger Does:
Avinger utilizes its Lumivascular imaging technology as a directional atherectomy procedure to treat PAD. It utilizes advanced OCT imaging technology to guide and assist the physician during the removal of plaque buildup from narrowed or blocked arteries.
OCT stands for Optical Coherence Tomography, which is a medical imaging technique used to obtain high-resolution, cross-sectional images of biological tissues.
During Avinger’s Lumivascular atherectomy procedure, a special catheter equipped with OCT imaging and a stainless-steel cutter is inserted into the affected artery. The imaging technology allows the physician to see inside the artery in real-time, providing a clear view of the plaque and the arterial wall. The cutter removes plaque and stores it in its nosecone to be safely removed from the artery thereby restoring blood flow to the affected artery.
Unlike traditional atherectomy methods that rely solely on X-ray images, Avinger’s Lumivascular atherectomy offers the advantage of direct visualization, which allows for a more targeted and precise removal of the plaque, minimizing the risk of damaging healthy arterial tissue.
Take Action:
If you or a loved one is suffering from the possibility of amputation, take action today. Find a doctor who performs Lumivascular procedures in your area. Lumivascular atherectomy allows your doctor to see inside of your arteries and safely restore blood flow in the affected artery. Improve blood flow in your arteries, find a Lumivascular doctor today.
Literature Cited
- Yuan, S., Levin, M. G., Titova, O. E., Chen, J., Sun, Y., Million Veteran Program, V. A., Åkesson, A., Li, X., Damrauer, S. M., & Larsson, S. C. (2023). Sleep duration, daytime napping, and risk of peripheral artery disease: multinational cohort and Mendelian randomization studies. European heart journal open, 3(2), oead008. https://doi.org/10.1093/ehjopen/oead008
- European Society of Cardiology. (2023, March 16). Short night-time sleep linked with nearly doubled risk of clogged leg arteries. ScienceDaily. Retrieved July 26, 2023 from www.sciencedaily.com/releases/2023/03/230316114126.html