Topics: Peripheral Artery Disease, Atherectomy, obesity, clogged arteries
Obesity increases a person’s likelihood of developing Peripheral Artery Disease.
What is Peripheral Artery Disease?
PAD affects almost 20 million people in the United States1 and over 200 million people across the globe.2 Peripheral Artery Disease affects a patient’s arteries that supply blood to their extremities. These arteries become blocked and obstructed which decreases healthy blood flow causing pain and cramping in the legs.
Obesity and PAD
While previous research has established that people with obesity are an at increased risk of developing coronary heart disease, a new study has found another link. This research has found that people with obesity are 1.5 times more likely to develop Peripheral Artery Disease (PAD) than people at a normal weight.3
"People with obesity are 1.5 times more likely to develop Peripheral Artery Disease"
This is why it is critical that doctors advise their patients with Peripheral Artery Disease and obesity to lose weight. However, this can be extremely difficult. PAD and obesity create a vicious cycle where it becomes very hard for patients to lose weight. These patients may have trouble walking due to the leg pain and cramping caused by Peripheral Artery Disease. This leg pain then makes it much more difficult for patients to stay active and lose weight. As the cycle continues, the more their legs hurt, the less weight they lose, the more their legs hurt, and so on.
 The link between obesity and PAD may also be due to diabetes. Diabetes is an obesity-related condition, and people with this condition are four times more likely to have Peripheral Artery Disease. In fact, 20% of all of the symptomatic people with PAD have diabetes.4
The link between obesity and PAD may also be due to diabetes. Diabetes is an obesity-related condition, and people with this condition are four times more likely to have Peripheral Artery Disease. In fact, 20% of all of the symptomatic people with PAD have diabetes.4
How to Prevent Limb Amputation from Obesity and Peripheral Artery Disease
Researchers have found that obesity leads to an increased risk of limb loss.3
Obese patients with PAD are at an increased risk of needing limb amputation. Patients who have diabetes may feel reduced pain because they experience peripheral neuropathy. Peripheral neuropathy is a term for the weak or numb feeling a patient feels in hands and feet. The reduced pain perception is caused by nerve damage.
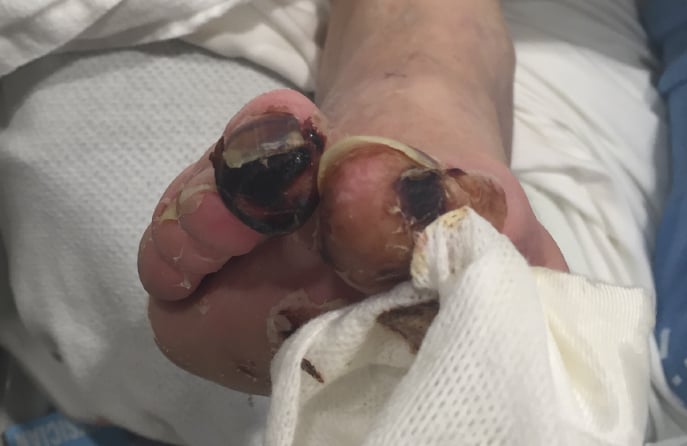
This means it’s highly likely that a patient that has obesity, diabetes and PAD will not notice the symptoms of PAD until the more painful symptoms appear. These very serious symptoms include ischemic ulcers and gangrene.
If these symptoms are ignored or not treated in time, patients run the risk of having their lower limbs amputated. Doctors recommend for patients with diabetes or PAD to check their feet each day for non-healing wounds and for early signs of gangrene.
Why Restoring Blood Flow is Important for Patients with Peripheral Artery Disease
If you have Peripheral Artery Disease, a Lumivascular atherectomy may be the best treatment option for you. The Lumivascular procedure is one of the latest technological advancement in atherectomy therapy. It comes equipped with a camera-like imaging fiber on the end of the catheter, that allows a physician to see inside the patients’ artery in real time as they remove the plaque that is obstructing the artery and preventing healthy blood flow.
Take Action:
- Patient Story: Bertha Ann Patient Story
- Learn more about Lumivascular atherectomy and Pantheris device
- Find a Lumivascular doctor in your area
Related Articles:
- 14 Fast Facts About Diabetic Foot Disease and Peripheral Artery Disease
- Diabetes and Peripheral Artery Disease
If you have found this article helpful, please don’t forget to share!
References:
- Yost, ML. THE ECONOMIC COST OF PAD, CLI & VENOUS DISEASE: HOW BIG IS THE MARKET? NCVH Annual Conference May 30, 2018.
- Fowkes, et al. Comparison of global estimates of preva¬lence and risk factors for peripheral artery disease in 2000 and 2010:a systematic review and analysis. Lancet 2013;382: 1329¬40.
- Hicks, et al. Associations of Obesity With Incident Hospitalization Related to Peripheral Artery Disease and Critical Limb Ischemia in the ARIC Study. J Am Heart Assoc. 2018 Aug 21;7(16)
- Murabito JM, D’Agostino RB, Silbershatz H, Wilson WF: Intermittent claudication: a risk profile from the Framingham Heart Study. Circulation 96:44–49, 1997